OPTICAL ASSESSMENT
A portable, non-invasive brain-imaging device uses light to “see” what the surface of the brain is doing while a person is taking a test or performing a task.
Wired for Recovery


Wired for Recovery
Projects to help military veterans who have lost limbs and those suffering from post-traumatic stress thrive in the collaborative environment of UT Arlington’s new Engineering Research Building. But ex-soldiers aren’t the only ones who’ll benefit from the partnerships forged in the state-of-the-art facility.
· Summer 2011 · Comment ·
Dung Mai wants to know why he struggles taking tests. The UT Arlington exercise science junior thinks the research of Alexa Smith-Osborne and Hanli Liu can help him find the answers.
“When I came back to school, I had some test anxiety,” says Mai, a Navy petty officer who served stints overseas in Bahrain and Jordan. “I thought it might be more than just anxiety, so this research helps me find out what my brain is doing, where I am in learning.”
Dr. Smith-Osborne from the School of Social Work and Dr. Liu from the Bioengineering Department are exploring better treatment for veterans suffering from post-traumatic stress disorder, traumatic brain injury, and other issues that hamper cognition. They believe that using a hybrid of testing and diagnostics will lead to better therapy and care.
Liu says the key is joining the psychosocial assessments with physiological testing. “That will provide better information for where people are in their ability to learn.”
They aren’t the only UT Arlington researchers delving into veterans’ issues.
Bioengineer Mario Romero-Ortega received a $2.2 million grant from DARPA, the research and development office for the Department of Defense, to further develop technology that will enable amputees to control and feel bionic limbs. The goal is to help the thousands of U.S. soldiers who have been wounded and lost one or more limbs by understanding why current peripheral nerve interfaces fail. Dr. Romero-Ortega hopes his neural interface will lead to a better prosthetic arm with more movement and even sensation.
VETERANS BENEFITS
Hanli Liu and Alexa Smith-Osborne assist veterans with cognitive problems.

Like Liu, Romero-Ortega works with researchers outside his department. One is mathematics Assistant Professor Yan Li, who specializes in biostatistics and biometrics.
Such interdisciplinary partnerships permeate the new Engineering Research Building. Other research in the 234,000-square-foot structure matches biologists with electrical engineering professors to detect viruses and fight pancreatic cancer, and bioengineers with physics professors to improve drug delivery systems for cardiovascular disease.
“To address today’s key medical problems, collaboration is essential,” says Ron Elsenbaumer, vice president for research and federal relations. “Not only does it foster complementary research, but, more importantly, the results are often better.”
“I think many of these projects will help countless veterans live more normal lives.”
BROAD IMPACT
Thousands of military veterans are taking advantage of legislation that helps pay for their college education. At UT Arlington, veteran enrollment reached 1,128 in spring 2011, more than double the number two years ago.
“Our researchers look at challenges and problems people face every day. Helping military veterans through University research is just part of who we are and what we strive to provide,” Dr. Elsenbaumer says. “I think many of these projects will help countless veterans live more normal lives.”
Research like Romero-Ortega’s offers hope for recent social work graduate Anthony Pone. “It’s like a bright light and gives us another option,” says the Army veteran and wheelchair basketball player, who uses a prosthetic and a wheelchair.
Yan Li and Young-tae Kim are part of an interdisciplinary team developing technology to help amputees control and feel bionic limbs.

Even though the research could greatly enhance veterans’ lives, broader populations—like those involved in accidents—also could benefit. Romero-Ortega became involved in nerve regeneration because a childhood friend from Mexico lost the use of her legs in a car wreck.
“I wanted to do something about it,” he says. “This work could eventually lead to solutions for people so negatively affected in car accidents.”
The research of Smith-Osborne and Liu also could extend beyond helping veterans.
“The much broader use would be for any head trauma victims to use this hybrid system of brain scanning and testing to show what is happening so they can make more informed decisions to support quality of life, and to show doctors what treatment is best for specific patients,” Smith-Osborne says.
Other projects using the technology are taking shape. Bioengineering Assistant Professor George Alexandrakis has received a $1.16 million National Institutes of Health grant to use the brain-scanning device in research on children with cerebral palsy.
“It will be broadly explored through different departments targeting other important applications,” Liu says.
SCANNING FOR SOLUTIONS
UT Arlington is the only university in the world with three cutting-edge optical brain-imaging devices to explore applications in cognitive sciences. The emerging technology uses light to scan the brain and lets researchers “see” brain functions without invasive procedures. A veteran’s forehead can be scanned while he or she sits in a chair and takes cognitive tests.
“To see what the surface of the brain is doing while a person is taking a test or performing some task can give us new insight for treatment and therapy,” Liu says. “Plus, this machine is portable and easier to use than functional MRIs. Our method does not require whole body confinement, making the subject more comfortable during the measurements.”
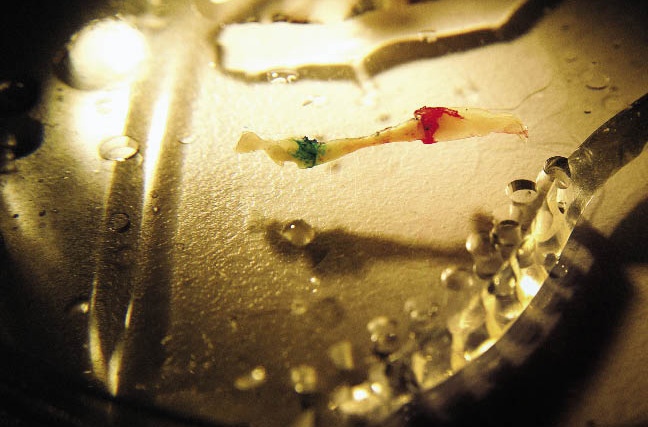
GROWING HOPE
Bioengineers are exploring how to regenerate nerves like this one colored in green and red to create a more reliable and stable prosthetic.
Smith-Osborne and Liu met through discussion groups at UT Arlington’s Southwest Center for Mind, Brain and Education, which explores connections between brain anatomy and physiology, cognitive neuroscience, educational philosophy, learning processes, and learning issues like dyslexia and attention deficits.
“I was looking for physiological testing, and Hanli said she had a portable, non-invasive brain-imaging machine,” Smith-Osborne says. “We started talking and decided to team up.”
“Rapid advances in engineering and cognitive science need to be translated to practical applications that people can use to reach their life goals.”
In 2007 Smith-Osborne founded the Student Veteran Project, a clinical intervention that offers free services to help veterans returning to college. Some were experiencing learning difficulties associated with the interactive effects of post-traumatic stress disorder and traumatic brain injury, as well as prior learning disabilities and co-occurring conditions such as pain.
“They were also having delays and difficulty in obtaining prior educational records and updated comprehensive cognitive and educational assessments,” Smith-Osborne says. “Scarcity of health resources may limit the availability of such assessments to the most severely injured veterans served in polytrauma centers.”
A private donation fund has been established to help pay for the assessments, which typically aren’t covered by insurance.
“We hope that the research testing leads to policy changes that will expand these types of resources for veterans,” Smith-Osborne says. “Rapid advances in engineering and cognitive science need to be translated to practical applications that people can use to reach their life goals.”
The program is open to all veterans.
“Of course, we love to have UT Arlington veterans and other North Texas veterans in the program, but we’re also available to serve all veterans all over the country who are considering going to college.”
A MOVING EXPERIENCE
Romero-Ortega’s work has national appeal, too. His $2.2 million grant is part of the RENET (reliable neural interfacing) program led by Jack Judy, program director of DARPA’s Microsystems Technology Office in Arlington, Va.
Robotic prosthetics have advanced from simple hooks in the 1850s to multi-finger, electronically controlled hands with 22 degrees of freedom. Modern devices closely resemble a human hand.
But neural interfaces are required to give amputees the most natural control and sensory perception. The process involves connecting the robotic prosthetic to the user’s nervous system, and current technology is unreliable.
Human arms are controlled through thousands of nerve channels that allow the limb, hand, and fingers to operate independently and precisely. The channels enable motion and sensory control.
By contrast, the most advanced neural interface in peripheral nerves for prosthetic arms uses six to eight channels and allows only simple movement without sensation. Neural interfaces implanted directly in the brain can provide hundreds more channels, but this requires surgery.
STRONG CONNECTIONS
Mario Romero-Ortega, right, and his team received a $2.2 million grant to develop a neural interface that better connects a robotic prosthetic to a user’s nervous system.

“What makes our research different is that we’re putting the neural interface in the limb itself,” says Romero-Ortega, who explains that the tiny interfaces allow the arm to interpret what the brain is telling it to do and the brain to interpret what the arm is doing.
About 90 percent of existing research in robotics and prosthetics focuses on the head, an approach known as brain-machine interface. Yet there is still no long-term, neural-electronic interface.
“Our research moves away from the head and into the appendage itself, looking for neural reliability and stability,” Romero-Ortega says. “It integrates the nerve into electrodes through nerve regeneration.”
In addition to Yan Li, Romero-Ortega’s team features Young-tae Kim, a UT Arlington bioengineering assistant professor who works with markers of inflammation, neurointerfaces, and histology. The project also includes Harvey Wiggins, president and founder of Dallas-based Plexon, and research scientist Edward Keefer; both bring expertise in neurophysiology, multi-electrode electrophysiology, and biochemistry.
The group is working to open up more of those channels to the arm through electrical and molecular engineering. The aim is to find clear signals and results that lead to clinically viable engineered systems with sufficient reliability and stability to last 50–70 years.
Romero-Ortega says initial testing shows the potential to open up hundreds of nerve channels to a prosthetic. These open channels would enable the body to control the prosthetic as if it were real, giving new functionality to amputees.
That’s exactly what Army veteran Pone, who lost his right leg in a car accident, hopes will happen.
“I think the research could give you more feeling, make you more independent. That’s what we’re all after.”
Web extra: Watch a video.
INNOVATION INSIDE
Researchers in the College of Engineering and College of Science collaborate in the 234,000-square-foot Engineering Research Building, which opened in January. Their projects include exploring cancer treatments, detecting deadly viruses, and improving the quality of life for older adults.




















This program is impressive and seems to be going at the right time for and by the right persons. Good to read about it.
The work reported here stresses the important requirement of researches in brain cognitive functions today, namely interdisciplinarity. I wonder if fMRI would be somehow and somewhere be involved in the project, or it has a chance to compare with that aspect of the research of the same subject simultaneously or at another moment. That link would be interesting if available.
I am referred here to read this nice report by Dr. Hanli Liu. She is definitely an intelligent and industrious research worker. She has a strong background of medicine tradition as her mother is an outstanding researcher in vaccine manufactory and three uncles/aunt and on grandpa are highly achieved medical doctors in their life career. I think she has been eventually come across to the physiological-medical aspect of bioengineering not out of no reason. She is the right person to play a role in this project and expect to have a significant contribution in the field.