Meet the Sims
UT Arlington’s high-tech Smart Hospital explores the most innovative ways to train health care professionals.
Students in UT Arlington’s Smart Hospital work on patient simulators like this one.
Sidney Logan felt queasy. It was probably a stomach bug or maybe food poisoning from all the adventurous dining he’d enjoyed on his trip to the Far East. After his 15-hour flight from Beijing landed at DFW International Airport, the 64-year-old began suffering waves of nausea and diarrhea. Seeking relief, he checked into UT Arlington’s Smart Hospital.
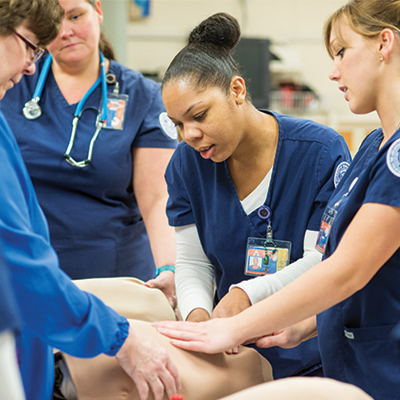
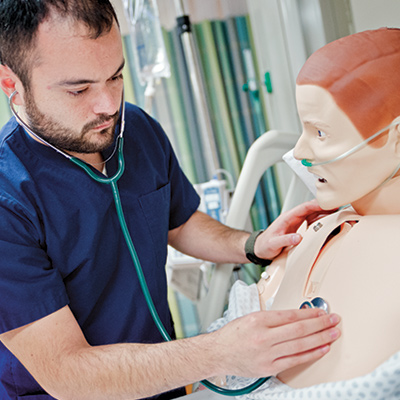
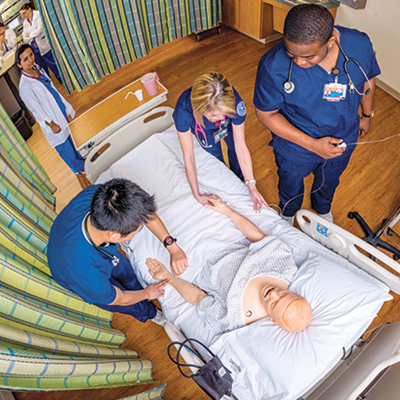
Hands-on training in the use of authentic health care equipment is part of the Smart Hospital experience for all students. State-of- the-science equipment helps students become more proficient.
When Amber, a student nurse, consulted his file at the beginning of her shift, she noticed a note from the previous nurse saying that, in addition to his nausea, Logan had complained of pain in his left calf.
Amber noted that her patient complained of nausea and leg pain and was already receiving nausea medication. His leg was slightly swollen, red, and warm to the touch. He had been sedentary for a long time on the flight and was probably dehydrated
She believed he may be at risk for developing a deep vein thrombosis (DVT), or blood clot in his leg, and decided to call the physician to report the change in Logan’s condition and her concerns about the possibility of a DVT.
Amber’s supervising professor, who had been evaluating her work, congratulated her on her performance, and Amber smiled in relief. She’s passed her exam.
Logan isn’t a human being. He’s a high-tech manikin who can simulate human breathing, pulse, speech, pupil reaction, and even bodily fluids. He’s one of over 40 manikins representing both genders as well as a variety of ages that are used in simulation education, research, and the development of innovative teaching methods. The Smart Hospital is a nationally recognized center for health care education using simulation techniques and hands-on teaching methods.
“Rather than ‘see one, do one, teach one,’ we actually allow students to perform a procedure and make an error on the manikin. This gives students the opportunity to see the consequences of their mistakes. In the clinical setting, instructors cannot allow students to make errors on real patients,” says Judy LeFlore, associate dean for simulation and technology in the College of Nursing and Health Innovation.
Changing classes
When it opened in 2007, the 13,000-square-foot Smart Hospital was at the forefront of the national trend of integrating more simulation into the nursing curriculum. Its equipment comes from three corporate partners: Laerdal Medical, which makes the manikins and other training devices; Hill-Rom, which produces hospital beds, room furniture, and headwalls; and CareFusion, which supplies equipment including IV pumps, respirators, and supply and medication dispensing machines.
By partnering with corporations that provide state-of-the-art technology, faculty can replicate real-world medical scenarios and tailor training to enhance hands-on learning opportunities.
But can simulation effectively replace the clinical hours traditionally required for nursing students to develop competency? In January 2015, the College of Nursing and Health Innovation received a $1.8 million grant from the Texas Higher Education Coordinating Board to identify the optimal simulation and clinical experience requirements for pre-licensure education.
The research will involve 1,700 students over 30 months and is a collaborative effort uniting UTA, three other nursing schools, the Dallas-Fort Worth Hospital Council Foundation (DFWHC), and several health systems including HCA North Texas Division, Baylor Scott & White Health, JPS Health Network, Kindred Healthcare, Methodist Health System, and Texas Health Resources.
“Hospital employers are interested in making the clinical portion of nursing education more efficient and effective when preparing nursing graduates to be ‘practice ready,’ ” says Sally Williams, director of the DFWHC Foundation Workforce Center. “This collaboration will make a significant impact on the preparation of future graduates entering the North Texas health care workforce.”
The project will begin by identifying specific skills, behaviors, and competencies students should be taught in areas such as pediatric and adult care. Then, data will be collected on study and control groups of nursing students as they progress through their clinical experiences, including an initial simulation experience.
In all, the researchers expect to gather more than 1 million data points before using the findings to make recommendations.
“UT Arlington is particularly qualified to lead this new research project because of our history of successful student outcomes, our emphasis on health research, and our groundbreaking work in simulation technology,” says Anne R. Bavier, dean of the College of Nursing and Health Innovation. “The results of this study will influence education and health care in Texas and the nation far into the future.”
Smart teaching
In July 2014, the National Council of State Boards of Nursing published a landmark study showing that simulation can effectively replace clinical hours in the hospital.
Researchers compared three groups of students: one that predominantly did clinical experiences with live patients with not more than 10 percent of clinical hours spent in simulation, one that replaced a quarter of their clinical experiences with simulation, and one that replaced half of their clinical experiences with simulation. All three groups demonstrated equal knowledge, competency, and critical thinking, suggesting that simulation is an effective substitute for clinical time with actual patients.
“The study validates that student outcomes are no different if clinical experiences are replaced by well-designed and executed simulated clinical experiences,” Dr. LeFlore says.
Unlike traditional clinical training, the Smart Hospital ensures that students are exposed to a wide array of scenarios. Faculty can use a manikin to simulate a rare malady instead of waiting for a patient with that particular malady to seek care. Practicing on a manikin lets students make, and learn from, mistakes—something that could never happen with real patients.
In a scenario designed to test students’ abilities in a specific medical situation, faculty in the control room down the hall manipulate the manikins’ vital signs, symptoms, and even voices. Via cameras in simulated hospital rooms, they watch the scenario unfold and adjust the manikins in response to the students’ actions.
The exercises are recorded so faculty can review them with students. LeFlore says the debriefing is equally as important as the simulation itself.
“If we use video, the students can see what they did and identify their own mistakes,” she says. “They can sort of disengage from the encounter and talk about how it felt and what they could have done better. That’s where the learning really occurs, when you walk away from it and a skilled instructor helps you think about what just happened.”
A Cast of Characters
UT Arlington’s Smart Hospital is a Laerdal Center of Excellence in Simulation with state-of-the-science human patient simulators from infants to adults. They can mimic human vital signs and a variety of symptoms from rumbling stomachs to mournful wails. Instructors can present a variety of scenarios to help students gain confidence as they build skills. Meet a few of the (simulated) patients.
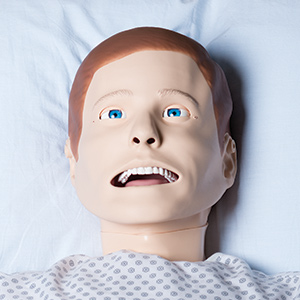
SimMan Essential. This simulated patient offers realistic breathing, eye blinking, and a human voice that can be prerecorded or transmitted wirelessly from an instructor. It can portray either gender and comes in a variety of skin tones.
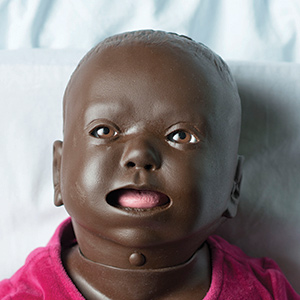
Nursing Baby. This simulator can present normal, bulging, and depressed fontanelles for assessment and normal and abnormal heart, breath, and bowel sounds for auscultation.

SimMom. This simulated patient can present a variety of birthing scenarios including breech delivery, eclampsia, shoulder dystocia, ruptured uterus, and post-partum hemorrhage. She also can be used as a non-pregnant female patient.
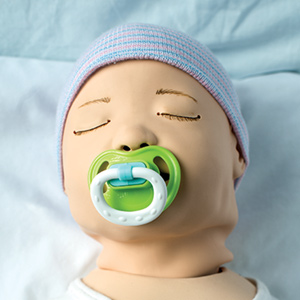
SimNewB. This high-fidelity baby simulator has an umbilical cord that can be assessed, cut, and catheterized for intravenous therapy. It can react to drug treatments and has a realistic pulse, breathing rates, and lifelike grunts that can be adjusted by the instructor.

SimJunior. This simulator represents a child around age 6 and can display a wide range of conditions, from a healthy, talking child to an unresponsive, critical patient with no vital signs.
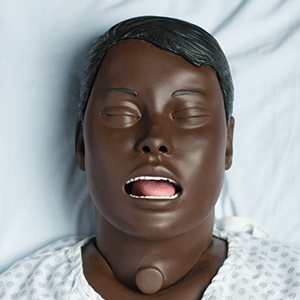
Nursing Anne. A moderate fidelity simulator, Nursing Anne is used to develop key skills from basic patient care to advanced nursing procedures such as wound assessment, recognition of breast disorders, and post-surgical mastectomy-care.
Remote possibilities
Research conducted by UTA faculty shows that simulation can also train professionals in the field—even those miles away.
“Because of the national focus on patient safety and quality, hospitals will be requesting that clinicians be able to demonstrate that they are competent in the procedures you say you can do,” LeFlore says. “But how do health care providers maintain competency if they don’t get the opportunity very often to practice those skills?” Simulations conducted across distance accomplish that, “especially for what we call high-risk, low-volume procedures.”
LeFlore is a pioneer in the latest technique called remote-controlled distance simulation, which creates the same kind of scenarios used to instruct students. But instead of the manikins and control room being nearby, they may be miles apart. By using manikins and related Laerdal software, LeFlore can run a simulation from the Smart Hospital at UTA for neonatal nurse practitioners at another site, whether across town or out of state.
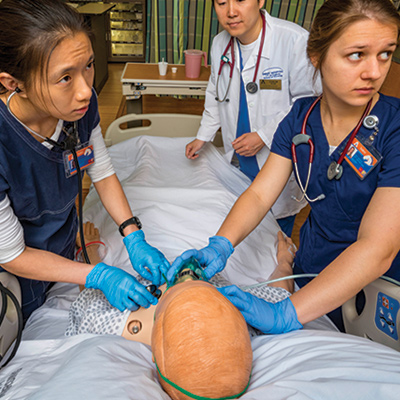

Dr. Judy LeFlore discusses various scenarios that can be programmed for patient simulators.
The technique first had to be tested to determine whether such remote simulations were possible. LeFlore and colleagues partnered with Pediatrix Medical Group, a division of the national medical network MEDNAX.
MEDNAX provides medical staff at 370 neonatal intensive care units nationwide and cares for almost a quarter of the neonatal intensive care unit patients in the country.
The company got involved because it saw simulation as a potential way to train its 700 neonatal nurse practitioners and validate their competency, says Debra Sansoucie, vice president for advanced practitioner programs at Pediatrix. It funded a feasibility test of a remote-controlled distance simulation of a neonatal care emergency, which LeFlore, from her computer in Arlington, ran for a team of Pediatrix clinicians at Cook Children’s Medical Center in Fort Worth.
The successful test and its implications for future training are documented in a paper published in the August 2014 issue of Clinical Simulation in Nursing by LeFlore, Sansoucie, Carolyn Cason, professor of nursing, Patricia Thomas, clinical assistant professor, and two more co-authors examining a 2012 simulation exercise.
The testing site was furnished with the SimNewB manikin, an infant patient simulator with capabilities including chest rise, pulse, and vocal and lung sounds, and the laptop that controls it with accompanying Laerdal software. Instead of someone at the hospital controlling SimNewB's behavior and response to treatment, LeFlore remotely accessed the SimNewB computer so she could run the scenario.
A second laptop on site sent footage of the event back to LeFlore by integrating with fixed and pan-tilt-zoom cameras using Laerdal’s SimView, an internet-based content management system that coordinated the video feeds and live-streamed them to the Smart Hospital.
Back at the Smart Hospital, LeFlore used one computer to control SimNewB and a second to watch the proceedings unfold. Just as in simulations that take place in the Smart Hospital, mere steps from the control room, LeFlore adapted SimNewB’s response to the interventions of the medical team in a hospital 30 miles away.
Continuing education
The success of the test demonstrated that simulation is a cost-effective training option for continuing education. LeFlore and Sansoucie are now in the third year of implementing a remote-controlled distance simulation program for practitioners using Pediatrix hospitals’ risk management data and credentialing requirements to choose scenarios that address critical needs.
It might be a premature baby, or (as in the test simulation) a baby with pneumothorax, a hole in the lung that causes it to collapse and the chest cavity to fill with air.
“We’re really focusing on what we call the low-volume, high-risk scenarios,” Sansoucie says. “Those are things you may not be exposed to that frequently. But when you are exposed, you need to know how to respond, and you need to respond rapidly.”
The UTA/Pediatrix partnership is the result of collaboration between LeFlore and Sansoucie, whose careers followed similar trajectories before they met at a conference in 2009. Both began as neonatal intensive care nurses, became nurse practitioners, and went on to teach at the university level.
Now that LeFlore, Sansoucie, Cason, Thomas, and their colleagues have demonstrated the effectiveness of remote-controlled distance simulation for practitioners, they’ve begun implementing such competency validation for Pediatrix clinicians across the country.
“We’re still in the infancy of this project, which I see just growing in importance as time goes by and as we’re able to embed it into our more than 140 practices across the country,” Sansoucie says.
“Hopefully, the research will be read by leaders of national organizations that can implement change,” LeFlore says, “and that will get the ball rolling.”
