In the face of a national shortage, UTA works to put the number of nurses back at a healthy level.
When Shirley Martin went to college, she never considered nursing because she had a needle phobia as a kid. But after she started the engineering program at Texas A&M, a friend encouraged her to become a nurse. The idea of taking care of people appealed to her, and when she enrolled at The University of Texas at Arlington to pursue her Bachelor of Science in Nursing (BSN), she knew she was where she was meant to be.
For the past 28 years, Dr. Martin has sat at children's bedsides as a pediatric nurse, doing her best to relieve their fears.
"I feel like I make a difference in the world," Martin says, a clinical instructor at UTA and a full-time pediatric perioperative nurse at Cook Children's Medical Center. "I have taken care of a lot of kids with needle phobias. Because of my own experience, I understand what a big deal that is."
Like Martin, many nurses feel called to the profession. It's a vocation oriented toward the whole patient, says Anne Bavier, dean of the College of Nursing and Health Innovation and president of the National League for Nursing (NLN). Nurses are sensitive to the emotional needs of patients and their families. They help patients learn how to use crutches and to understand when and how to take their medication. They can help patients address such daily life issues.
UTA is the top producer of baccalaureate-degreed nurses in Texas.
In fact, a recent Gallup poll ranked nursing as the nation's most trusted profession.
However, nurses often don't have the time to follow up with patients to make sure all those additional needs are met. Facing a rising nursing shortage, nurses at hospitals and other health facilities often find there aren't enough of them to go around.
To address the shortage, the Institute of Medicine published a report in 2010 outlining five areas that must be confronted to ensure the health care system will be sufficiently staffed with fully educated nurses. The recommendations included allowing nurses to practice to the full extent of their education and training; promoting baccalaureate and advanced degrees; allowing nurses to lead in the fields of health care policy, research, and translating research into evidence-based improvements to the practice; promoting diversity; and improving data collection on health care professionals regarding whether they work and what roles they fill.
UTA's College of Nursing and Health Innovation—the largest nursing program in Texas and the largest nonprofit nursing school in the country—rose to the challenge. UTA has created pathways to help more nurses further their education. Technology is playing a big role in making that happen, with both online programs and simulated training experiences, allowing nontraditional and nonlocal students opportunities to earn nursing degrees. The College also offers two doctoral nursing degrees, so nurses wanting to further advance their knowledge have the option to pursue research and science or specialized practice and leadership in the field.
While there will always be more work to do, UTA continues confronting the challenge head-on.
The nursing shortage
It's been a problem for decades, and it could get worse. The U.S. Census Bureau reported there were more than 46 million people age 65 or older as of 2014. By 2024, the youngest baby boomers will reach their 60s, continuing to burden the health care system with the chronic illnesses that comes with old age. And not only is the general population graying, so is the nursing workforce. The vast majority of nurses are female, and many entered the field decades ago when women had fewer career options. Today, more than half of registered nurses are 50 or older, and the average age of Texas nurses is 45. As more RNs reach retirement, the shortage may increase.
The employment of RNs is expected to grow 16 percent by 2024 according to the Bureau of Labor Statistics, a much faster rate than other occupations. That growth will put the number of new nursing jobs in the millions.
But it's not a lack of women and men desiring to become nurses that will cause jobs to go unfilled. A critical component of addressing the shortage is the ability of colleges and universities to prepare enough nurses to fill those vacancies. The two biggest hurdles these institutions face, Dr. Bavier says, are too few faculty members and not enough clinical sites for students to gain the hands-on experience they'll need in the field.
The first problem also stems from age: The American Association of Colleges of Nursing (AACN) reported in 2014 that the average age of doctorate-holding faculty is older than 50, and older than 60 for full professors. Master's degree-holding faculty are, on average, older than 50 as well. As faculty retire, the shortage of educators may also rise.
This problem presents a catch-22: The fewer faculty there are, the fewer students can be admitted into nursing programs. Then schools aren't able to graduate as many students, which results in fewer nurses who can become faculty members in the future.
The second issue compounds the problem. The more students enrolled in nursing programs, the more clinical sites are needed to complete their degree. Too few clinical placements limit the number of students who can be admitted into nursing programs. Thus the paradox starts again.
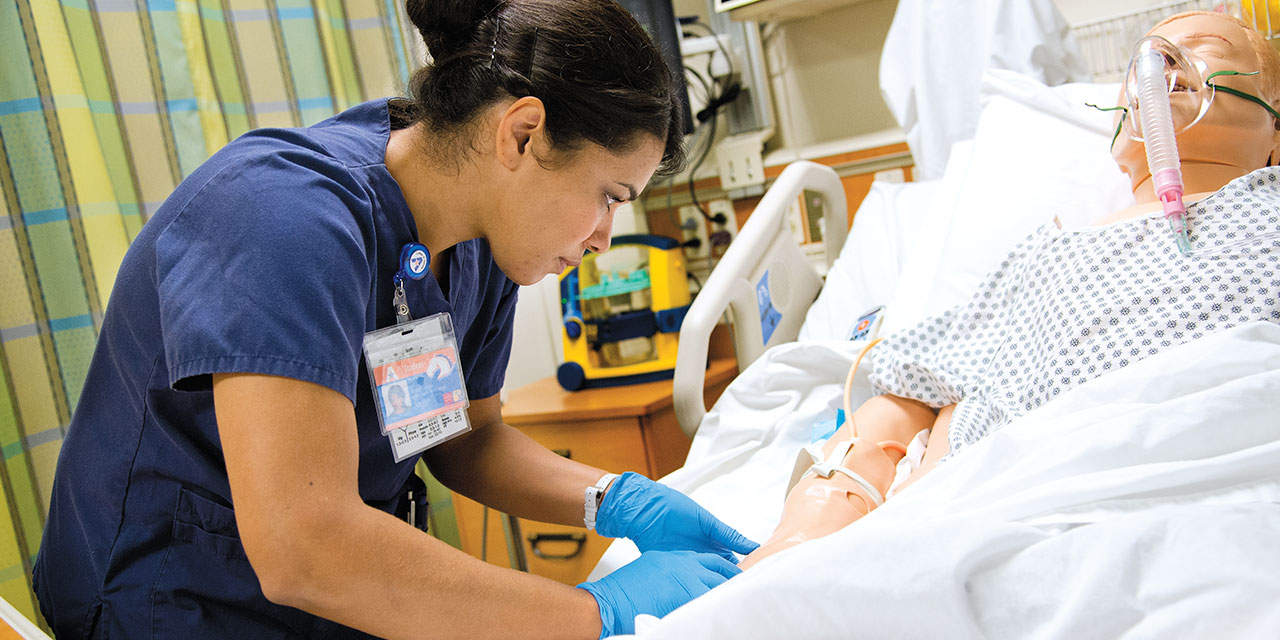
A student works with a manikin at the Smart Hospital.
RESPONDING TO THE PROBLEM
Along with other universities across the country, UTA also faces the task of finding enough doctorally prepared faculty to educate the number of students who apply. Nationally, almost 70,000 qualified applicants were turned away from nursing schools because there weren't enough faculty to teach them, according to the 2014 AACN report.
To combat the problem, the College turned to technology nearly a decade ago. The College offers numerous online courses, allowing faculty to teach more students without overcrowding classrooms. Simulated clinical experiences cut the number of hours students need to spend at hospitals, therefore reducing the burden on facilities that provide hands-on training. As a result, UTA accommodates more than 13,000 students in its nursing program and is the top producer of baccalaureate-degreed nurses in Texas.
UTA continues to broaden its online curriculum. The College has offered the BSN and some Master of Science programs online for years, and in March, several additional nurse practitioner degrees were added—allowing more students to earn advanced degrees in rural areas and out of state.
The online programs are accelerated, meaning that instead of 16 weeks of coursework, these classes take only five to 10 weeks. The benefit for students is the ability to graduate sooner, but the University does not sacrifice excellence for speed.
"The quality and content are the same, just delivered differently," says Judy Leflore, associate dean for simulation and technology, who also oversees the graduate nursing program. "We use the same metrics to evaluate online and on-campus programs."
Dr. Leflore stresses the accelerated online classes aren't for everyone. Because students must devote 15 to 20 hours per week to their academic studies, she recommends they not work at all or only part time if absolutely necessary.
Online classes serve another purpose as well. In addition to allowing more students to enroll, they also provide access for distance learners, especially those wanting to pursue advanced degrees.
"The shortage of nurses varies by geographic region of the country and of Texas," says Beth Mancini, the College's senior associate dean for education innovation, who oversees undergraduate studies. "In Houston and the Dallas-Fort Worth metroplex, the shortage isn't as bad because there are lots of schools. It's worse in rural areas, where shortages can be very high."
For that reason, she says, averages and generalizations of statistics obscure the severity of the shortage in underserved regions. With online classes, students can earn a degree from where ever they're located, increasing the likelihood they will remain and practice in those underserved areas.
Dani Dillard, an online student who expects to earn her BSN in December, lives in Argyle, Texas, about an hour's drive from UTA. In addition to her coursework, she works part time and cares for her family, leaving little room for a long commute to school. But she says she feels just as close to her professors as she would in on-campus classes.
"Many supportive structures help online students feel connected and supported," says Dillard, who plans to continue working in a pediatric emergency department. "You feel as if you're getting an in-person education. It takes dedication and commitment, but the educators are with you every step of the way to help you achieve your goals."
UTA professors emphasize the importance of strong relationships with students in the online setting.
"I became a faculty member when online education was exploding, and with the change in delivery mode comes the need to identify mechanisms to keep students feeling they are part of a larger community of learners," says Patricia Thomas. She earned her Ph.D. from the College in 2011 and now teaches neonatal nurse practitioner courses at UTA full time. "In addition to discussion forums, I utilize web conferences, wikis, Blackboard instant messenger, and journaling to facilitate communication in the online courses I teach."

Students learn emergency care during a field training session.
hands-on training solutions
Because UTA increased its ability to enroll more students, it also had to find a way to accommodate the need for clinical training. Again the University turned to technology, with a Smart Hospital that includes simulators for students to practice their skills before working with real people. This groundwork reduces the number of hours needed in clinical placements.
"With a simulated experience, you don't have to touch a patient the first time you try a new skill," says Beverly Malone, CEO of the NLN. "It's like with pilots—you can crash the plane without anyone getting hurt. With the virtual simulation, you've experienced all types of scenarios by the time you get to a hospital. You have also had the opportunity to reflect on what you did wrong without anyone losing their life."
During simulations, students encounter events such as a patient going into cardiac arrest or having a baby. Such experiences prepare them to make good judgments during clinicals, Dr. Malone says.
The Smart Hospital also integrates technology into the curriculum. UTA was one of the first schools to build a virtual hospital setting which includes emergency, surgery, adult ICU, neonatal ICU, pediatric care, and delivery rooms.
In the beds lie programmable manikins—mannequins that talk, get fevers, vomit, deliver babies, and simulate many other human bodily functions. As the nurses care for their patients, faculty observe from a one-way window and remotely adjust the manikins' settings to respond to the students' actions. While online students don't have access to the Smart Hospital, the facilities where they earn their clinical hours offer simulation opportunities.
"This technology doesn't replace clinical experience, but it makes it go more smoothly," Dr. Mancini says. "When the students get into the clinical experience, they don't need as many exposures to a situation to demonstrate competency. They can interact more confidently with real patients."
UTA also has established partnerships with hospitals to create flexible schedules for clinical hours. Working weekends or evenings allows students to log the same number of hours in fewer months. These partnerships also extend to underserved areas, allowing long-distance students to avoid time-consuming commutes.
accelerating advanced education
Nurses who advance their education bring many benefits to the workplace and the health care system, according to a 2013 report by the Robert Wood Johnson Foundation. Improved patient outcomes have been linked to nurses with bachelor's degrees or higher, the report found.
UTA's nursing programs make it easier for working nurses to advance their education, says Ceil Flores, assistant dean of the College of Nursing and Health Innovation. The RN-to-BSN and RN-to-MSN programs allow licensed, practicing registered nurses to earn a degree using their professional working experience as credit for clinical hours. UTA also offers MSN-to-Ph.D. and BSN-to-Ph.D. options to facilitate advancement to the doctoral level.
UTA's nursing programs make it easier for working nurses to advance their education.
The Doctor of Nursing Practice (DNP) is also a doctoral degree, but instead of focusing on research, it aims to prepare nurses for leadership, health policy, and specialized clinical practice. In some cases, nurses with DNP degrees opt for careers in academia.
Bavier stresses the importance of determining which doctoral course is appropriate for students wishing to pursue terminal degrees.
"People go into nursing with a passion for helping others," she says. "Part of what we do in the admission process is help people determine how to make an impact in a way that's most aligned with their life goals."
ATTRACTING teacher-researchers
While the number of nurse educators is low, the number of faculty members with doctorates is lower still. Among full-time nurse educators, only about 33 percent hold either a Ph.D. or DNP, according to a 2015 NLN report. In Texas, less than one percent of nurses hold a doctorate, the Texas Center for Nursing Workforce Studies reported in 2015.
Salary remains a barrier to enticing nurses into the classroom. The average salary of a nurse practitioner is more than $90,000, according to a 2014 American Association of Nurse Practitioners report. But the average salary for a master's-prepared assistant professor is less than $75,000.
It's a problem for universities across the country, and Mancini says finding money to hire new faculty remains a challenge for UTA. But the University is still moving forward. The administration has provided funding to make new hires for the past three years, allowing about 10 professors to be added to the faculty, Bavier says.
Some educators, like Martin, are drawn to expanding evidence-based practice in nursing. Even before she was employed at UTA, she led a scientific study theorizing that children could be positively influenced by therapeutic suggestions while under anesthesia. She received funding of more than $50,000 to conduct her study on children who had just received a tonsillectomy, a procedure that often caused young patients to wake up screaming in pain.
"Patients are still sleeping under anesthesia, so we used that window of time to speak soothing phrases to the child," Martin says. "We discovered that intervention significantly lowered pain scores 30 minutes after removal."
Now, in addition to her full-time job at Cook Children's Medical Center, Martin teaches an online course and continues her research interests, including postoperative pain in children, bio-behavioral interventions in the perioperative setting and obesity in children.
A versatile career
Besides getting to conduct original research, there are other reasons nurses decide to earn advanced degrees and go into teaching. Some nurses feel burned out by the stress of the hospital, and they may prefer more consistent working hours with weekends and holidays off. Many also enjoy educating future health professionals.
"I love getting to mold the next generation of nurses and watch the transformation from the first day you meet them to the last day after clinical," Dr. Flores says. "They blossom."
Mancini, with over 40 years' nursing experience and 13 as an educator, agrees. "That's one of most wonderful aspects of nursing—you can do all sorts of things," she says. "As a nurse, I loved my job because I could make an immediate impact. As an administrator, I made an impact by leading nurses who are caring for patients. Now as an educator, it's the best job in the world. The faculty are teaching nursing students who are going to go out and provide that care that I used to give. I've loved each aspect of being a nurse."

