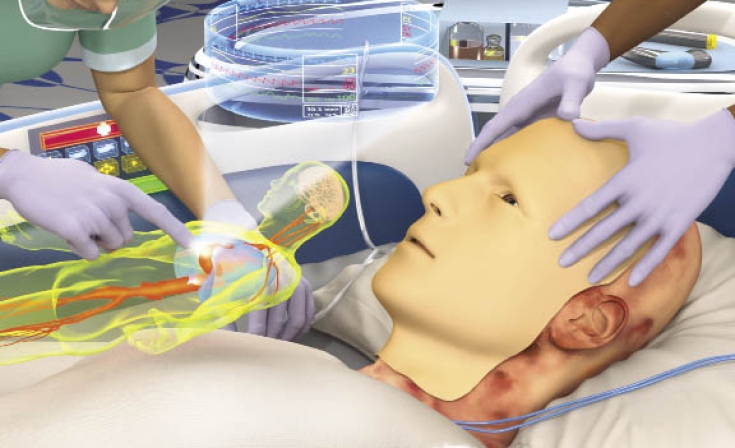
Biomask, 2025
Spring 2011 · Comment ·
Dealing with serious burns is a challenging medical problem, but researchers at UT Arlington’s Automation and Robotics Research Institute (ARRI) are making progress treating the deep facial burns often suffered by soldiers. In collaboration with the U.S. Army Institute of Surgical Research at the Brooke Army Medical Center in San Antonio, the approach involves a “biomask.” ARRI research scientist Eileen Moss calls it a paradigm shift in treating facial injuries. “The biomask consists of layers of flexible, biocompatible polymers embedded with arrays of active electrical and mechanical components,” Dr. Moss explains. “The array configuration allows localized activation of treatment to be applied to different parts of the wound as needed.” Current treatment involves removing damaged areas followed by grafting. Sometimes the outcomes are good, but the procedure also may result in deformities, speech problems, and scarring. “At this point we are far from any off-the-shelf composite tissue replacement that would mimic the suppleness and color of native facial skin,” Moss says, noting that there are additional problems with immunosuppression and with finding “like with like” donors. ARRI’s experimental biomask would utilize a network of microvalves and microfluidic channels to apply sub-atmospheric pressure to the facial surface. The mask would monitor the wound with assorted sensors and provide instant feedback. It also would adapt to the four basic stages of treatment: wound bed preparation, dermal replacement, epidermal overlay, and soft tissue augmentation. It’s a complex medical problem, but ARRI’s researchers believe the biomask will result in improved facial skin quality, fewer overall operations, and an earlier return to function or duty.